Critical Environment Reporting
Customer Requirements & Value
Overview
The purpose of this page is to explain how hospitals are using PointMatter to maintain control of their environments and comply with regulatory requirements.
The first sections cover the customer requirements and includes information on regulatory requirements. Later the document describes how the PointMatter system is used by customers to save time, money, and ensure the safety of staff and patients.
If you have any questions, please contact LogicMatter at partner@logicmatter.com.
Customer Requirements
Hospitals, medical clinics and pharmaceutical labs must have “control of their environment”. This is a regulatory requirement and safety concern. However, the exact engineering specifications of “control of the environment” are not defined by regulatory agencies.
It is up to the facility to define how it has control of its environment and to defend its methodologies to prove it has control.
LogicMatter developed the Critical Room report so hospitals, laboratories, manufacturing and other organizations can demonstrate control of their environment.
Value of Critical Room Report to Customers
The PointMatter Reporting Solution’s Critical Room Report is an integral part of a healthcare provider’s environment of care plan. It is used to demonstrate that an organization has control of its environment.
The Critical Room Report:
-
- stores all regulatory standards that the healthcare provider uses for critical environments
- defines each critical environment that is to be tracked
- assigns regulatory standards to each environments for the purpose of reporting
- provides a consistent, professional reports
- shares the reports with all stakeholders including facilities, administration, department heads, and EC management on a scheduled basis to inform all stakeholders
- is used to quickly demonstrate regulatory compliance to auditors
Using the Critical Room Report from PointMatter demonstrates to auditors that a hospital closely monitors its environments and has a robust system to follow their environment of care.
Environment of Care Management Plan
Each healthcare facility must have a plan for its Environment of Care (sometimes called EC). This plan covers six areas:
- Safety
- Security
- Hazardous materials and waste
- Fire safety
- Medical equipment
- Utilities
With regards to a facility’s HVAC system, the medical facility needs standards for each of its critical environments such as operating rooms, ICUs, and sterile processing and decontamination rooms.
The standards that are applied to each critical environment are not spelled out by the accreditation organization. Instead, the medical facility defines its standards based on best practices for its critical environments. The EC plan should document why these standards are used.
Standards for specific room types are published by ASHRAE, FGI, AIA and others. An organization may use a combination of standards from these engineering associations for each specific room type.
Standards may also be defined by the healthcare organization. For example, the minimum temperature for an operating room in most standards is 68 degrees Fahrenheit. A hospital could specialize in a type of surgery that requires a lower temperature. If this is the case, the hospital should document why it uses a lower temperature standard.
Regulatory Agencies
Medical facilities are regulated by the Department of Health, accreditation groups such as The Joint Commission, and in some cases the FDA. Facilities are audited by these agencies on a regular basis. If a facility produces therapeutics (many hospitals do), then the FDA will also inspect the facility.
The Joint Commission is a non-profit organization that accredits more than 22,000 health organizations and programs. Its mission is to “To continuously improve health care for the public, in collaboration with other stakeholders, by evaluating health care organizations and inspiring them to excel in providing safe and effective care of the highest quality and value“.
Accreditation by the Joint Commission is recognized by government agencies such as Medicaid and Medicare. Failure to be accredited would mean the facility would not be eligible for payments from these government agencies. This is a significant financial risk.
A medical facility can also be audited by the Centers for Medicaid and Medicare Services, or CMS. Normally CMS would rely on the Joint Commission for audits. CMS will check a facility to make sure the audits are being performed correctly.
Some states do not recognize the Joint Commission (Oklahoma, Pennsylvania, and Wisconsin). There are other healthcare accreditation agencies that accredit healthcare organizations in these states.
Audit Example without PointMatter
An audit by the Joint Commission is a high stakes event for healthcare providers. During the audit, the auditor will make sure the healthcare organization has a well defined environment of care plan for its critical environments and that this plan is being followed.
An auditor will ask a healthcare administrator:
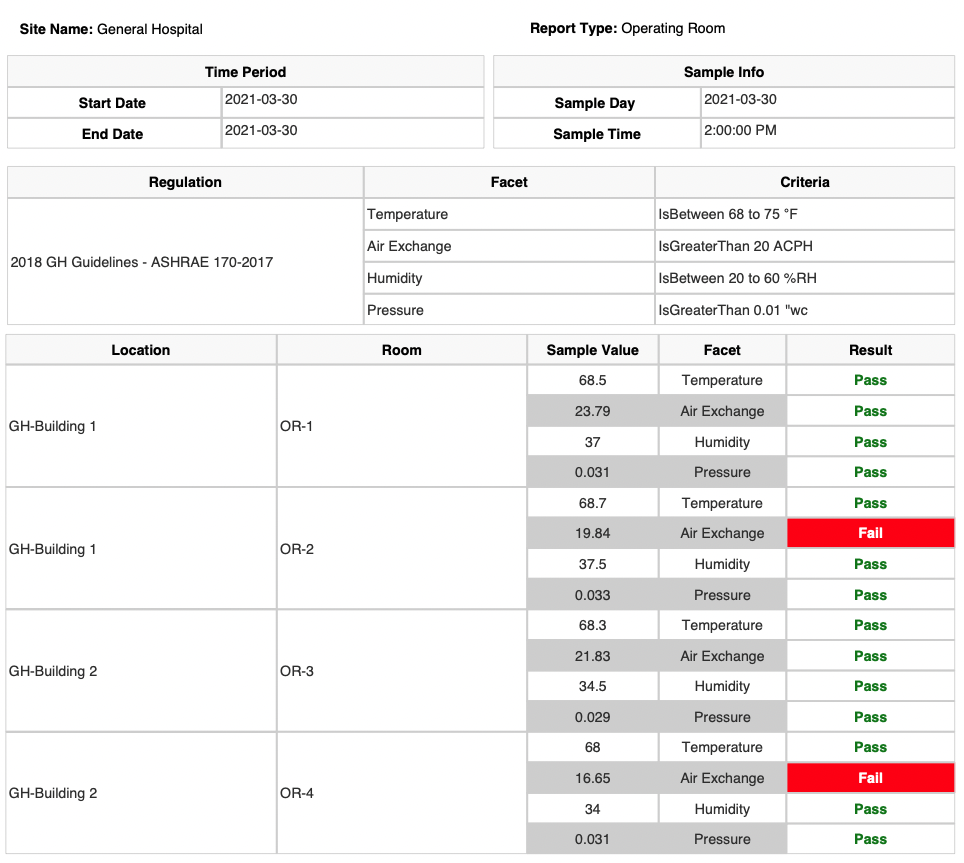
Show me the temperature, humidity, air pressure, and air changes per hour for Operating Rooms 1 and 2 for January 11 through 15 of 2022
Without a tool like the PointMatter Critical Room Report, the administrator would first call the facility group, find the right person, ask for the information, the information would be retrieved from the building management system’s database, put in a spreadsheet, and then reconciled with the EC plan. This could take days or more.
If the information is not complete or not readily available, the auditor will ask more questions to determine why the healthcare organization cannot produce this information quickly. It would be apparent that key stakeholders in an organization are not informed if the environment of care is being met on a regular basis. It demonstrates that an organization does not have adequate control over its environment.
This can become a very time consuming and expensive process if the healthcare provider is unprepared. It could lead to the temporary shutdown of the facility, loss accreditation and millions of dollars in lost revenue.
Audit Example with the PointMatter Critical Room Report
An auditor will ask a healthcare administrator:
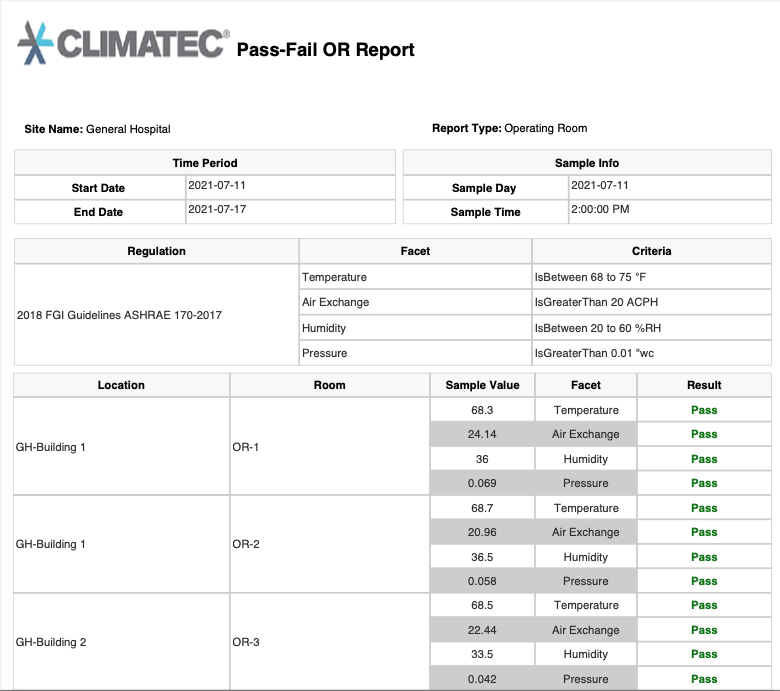
Show me the temperature, humidity, air pressure, and air changes per hour for Operating Rooms 1 and 2 for January 11 through 15 of 2021
The administrator would run the Critical Environment app while meeting the auditor. They would select operating rooms 1 and 2 and then enter the date range as January 11 through January 15, 2021. In seconds they are able to show the auditor a professional report.
The administrator can then explain that these reports are shared with the department heads on a weekly basis. The standards are listed in the report and should also be listed in the Environment of Care Management plan.
Quickly providing the information requested demonstrates that a healthcare provider has control of its environment. The audit of its environment could end in minutes instead of weeks.